Skin Cancer Can Occur Under Your Nails and Inside Your Mouth – Here’s How to Reduce Your Risk
Get the inside scoop on skin cancer prevention from leading doctors and a three-time skin cancer survivor.
In 2018, I wrote my first article for Beautytap about my first skin cancer surgery. Fast forward five years, and I’ve now had three surgeries and 25+ biopsies. I’m cancer-free today (*knocks on wood*) but that might not always be the case.

Before and After of Tracy Teel after Mohs Surgery and Erbium Laser
Skin cancer is rarely caused by what you’ve done lately, so I’m sharing what I’ve learned as well as expert guidance from Stanford-Educated, Board Certified Dermatologist Dr. Tess Mauricio and Facial Plastic Surgeons Dr. Ron Moy and Dr. Lauren Moy.
Skin Cancer Risk Factors
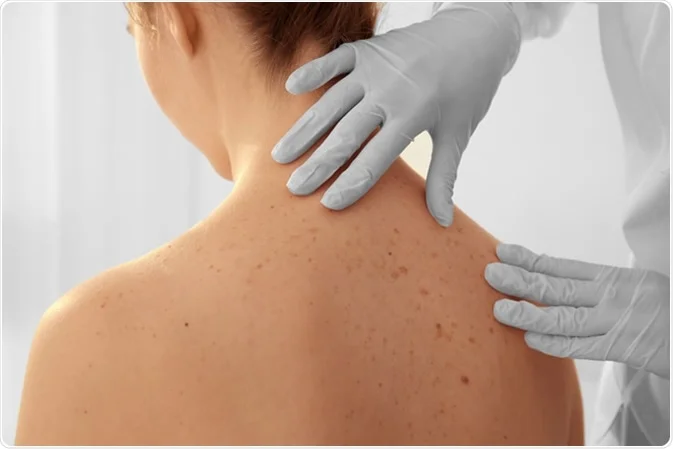
How often do you visit your primary care provider? If you’re relatively young and healthy, you probably only go to the doctor when you’re sick. But when it comes to staying ahead of skin cancer, it’s important to know your risk factors early on. According to Dr. Tess, you are at the highest risk if you have the following:
- Fair skin (rarely tans but burns easily with sun exposure)
- History of bad sunburns as a child and teenager
- Family history of skin cancer
- Lots of moles and growths on the body.
Having several of these risk factors means building a relationship with a dermatologist in your teens or age 30 at the latest, even if your risk is minimal.

Dr. Lauren Moy and Dr. Ronald Moy
People of Color Are Still at Risk for Skin Cancer
Think your melanin-rich skin tone (Fitzpatrick III – VI) eliminates the risk of skin cancer? Think again. Even people with darker skin tones can develop skin cancer. While rare, Dr. Tess has “diagnosed patients with skin cancer who were non-Caucasian.” Research has shown that skin cancer outcomes for people of color (POC) are often worse because cancerous lesions are less likely to be diagnosed early.
Part of this disparity hinges on a common fallacy that “darker skin is protected from the sun’s harmful rays.” Melanoma, for example, often surfaces in non-sun exposed areas of the body, like the soles of the feet and palms of the hands. It can also occur under the nails, on the genitals, and inside the mouth – areas that are rarely caught via self-examination. For example, in Health Disparities and Skin Cancer in People of Color, the authors note that “Acral lentiginous melanoma (ALM) can resemble a traumatic injury or fungal infection.”
Create Your Own Mole Map to Document Changes
Observing skin-related change isn’t easy, and no one remembers everything perfectly, so don’t rely on memory when it comes to what you observe on your body. One of my favorite tools is a mole map. After my first basal cell carcinoma (BCC) surgery, I downloaded this helpful diagram from the American Academy of Dermatology to keep my own records in between derm visits. Using a mole map is easy. Simply record what you see, and you’ll have an accurate reference to compare new findings to and to share with your dermatologist.
Mole Mapping
Learn the ABCDEs of Skin Cancer Self Examination
When examining your skin, experts like Dr. Tess recommend following the ABCDE method to help determine if something looks suspicious:
A – Asymmetry is a warning sign. The two sides of a healthy mole/spot usually look alike.
B – Border should be smooth, not jagged.
C – Color should be the same throughout.
D – Diameter should be smaller than 6 mm (pencil eraser) but some skin cancers are smaller. My melanoma was 5 mm.
E – Evolution. Troublesome symptoms include changes in color, shape, or size.
P.S. Healthy moles don’t itch or bleed.
“If you find any of these signs when inspecting your moles and growths,” Dr. Tess says to “see your Dermatologist right away. [Having] any of these signs does not automatically mean you have skin cancer, but it means you must be evaluated for a possible skin biopsy.”
Some Forms of Skin Cancer Are More Common Than You Think
One of the most common forms of skin cancer is basal cell carcinoma (BCC). According to the American Cancer Society, “about 5.4 million basal and squamous cell skin cancers are diagnosed each year in the US (occurring in about 3.3 million Americans, as some people have more than one). About 8 out of 10 of these are basal cell cancers.”
Surgical Options Vary, So Do Your Homework
Dealing with a cancer diagnosis is frightening, so make sure your dermatologist or surgeon explains the surgical approach thoroughly … and ask lots of questions. I’ve had an in-office excision, an out-patient hospital procedure, and Mohs surgery, so I understand that “one size fits all” doesn’t exist in the realm of skin cancer. The one thing all three surgeries have in common is the inevitability of scarring, which is why Dr. Ron Moy is the only person I trust with my face.
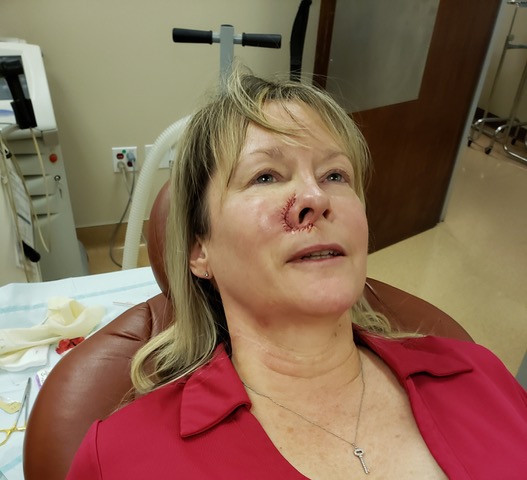
Tracy Teel during Mohs Surgery
Mohs Surgery Should Be Handled By a Specialist
Unlike an excision, which often removes excess tissue in an attempt to achieve clear margins around the existing cancer, Mohs micrographic surgery is a tissue sparing surgery. Mohs is named after Frederic E. Mohs who pioneered the technique. In short, the goal is to achieve “the highest cure rate while sparing healthy tissue and leaving the smallest possible scar.” If you’re diagnosed with any type of skin cancer, it’s best to imagine the visible cancer as the tip of the iceberg. There’s no way of knowing how much tissue damage resides below the surface, so if your cancer is in a cosmetically important area, like your face, Mohs is the best option. The Mohs surgeon will remove the cancer in small layers, analyze the tissue immediately, and remove additional tissue until all the margins are clear.
In my case, my cancer required the removal of two layers of tissue in the center of my cheek. Dr. Moy’s reconstructive expertise enabled him to pull the tissue toward the center of my face, so the wound would close in the natural shadow of my nose. I’m 1000% certain that I would have been disfigured had I allowed someone less experienced to perform my procedure. But don’t assume your dermatologist has received this training. “Not all facial surgeons are trained to do Mohs,” says Dr. Moy. “Only board-certified dermatologists who are medical doctors and undergo a fellowship are trained to perform Mohs surgery and reconstructive surgery.” He adds, “Every practice is built and run differently, but every patient has the right to know and ask who is performing what procedure on them and their experience level.”
Know Your Options for Scar Remediation and Preventative Treatments
Once you’ve tackled your cancer situation and have healed to your doctor’s satisfaction, you can start discussing treatments to minimize the appearance of your scar. According to Dr. Ron and Dr. Lauren, “Scar remediation or revision depends on what the scar texture/color is, how the wound was closed initially, where it is on the body, and many other factors. [Patients are] usually advised to wait 4–6 months to consider surgical treatment, but patients can also consider other treatment options that range from injections, lasers, dermabrasion, etc.”
Since my Mohs scar is on my face, I opted for a fractionated Erbium laser treatment 10 months after my Mohs surgery … but not just for cosmetic reasons. Drs. Moy explained, “There is also recent data that shows resurfacing lasers such as 2940 nm [Erbium] and 10600 nm [CO2] can also help decrease pre-cancer and non-melanoma skin cancers.” These types of treatments aren’t usually covered by insurance, but the benefits far outweigh the cost as far as I’m concerned. So much so, that I have another Erbium laser treatment scheduled later this year.
A Few Topicals and Supplements That Are Worth Using
Beyond sunscreen and UPF clothing, there are promising skincare products as well as oral supplements that play a role in lowering the possibility of future skin cancer if you’re at high risk like me. “Oral supplements, such as nicotinamide can help decrease pre-cancers and some non-melanoma skin cancers by 30%.” Dr. Ron and Dr. Lauren also recommend topical DNA repair enzymes. I’ve opted for the trifecta approach and am keeping my fingers crossed that my most recent skin cancer surgery will be my last.
~ ~ ~
If you want to know more about the Erbium laser treatment, stay tuned to your Beautytap editorial feed for an inside look at what it entails and why it’s officially part of my yearly skincare regimen.
Loading...